Chiropractic and physical therapy demand continues to grow in 2026 as patients increasingly seek non-invasive treatment for chronic pain, sports injuries, musculoskeletal conditions, and post-surgical recovery impacting over 126 million Americans annually. At the same time, reimbursement is getting tighter. Medicare audits (including TPE reviews), stricter commercial payer authorization rules, and AI-based claim scrubbing systems are now flagging errors before payment.
High-denial states like Texas, Florida, California, New York, Illinois, and Pennsylvania continue to face increased scrutiny in rehab billing. Small errors in CPT coding, ICD-10 specificity, modifiers, authorizations, or documentation can quickly result in denials, delays, and revenue leakage.
This guide highlights the key 2026 updates in chiropractic and PT billing, including Medicare rules, coding requirements, modifier compliance, denial risks, and the impact of AI in revenue cycle management.
Why Chiropractic & PT Billing Is More Complex in 2026
Chiropractic and physical therapy billing is becoming more challenging in 2026 due to value-based reimbursement models, stricter payer rules, and AI-driven claim review systems. Insurance carriers and Medicare contractors now analyze coding accuracy, modifier usage, treatment frequency, medical necessity, and documentation consistency more aggressively than ever.
As a result, claims are increasingly denied for issues such as:
- Missing or incorrect modifiers
- Insufficient medical necessity documentation
- Unsupported ICD-10 coding
- Authorization failures
- Incorrect timed therapy coding
- Incomplete progress notes
- Maintenance therapy billing issues
Many denials begin long before claim submission during eligibility verification, authorization tracking, documentation review, and claim scrubbing workflows.
This challenge heavily impacts chiropractic clinics, physical therapy providers, orthopedic rehabilitation centers, sports medicine practices, and pain management groups. As payer requirements continue evolving, rehabilitation providers increasingly need specialty-focused revenue cycle management instead of general billing support.
2026 Medicare Chiropractic Billing & Regulatory Updates
Medicare chiropractic billing continues to be one of the most closely monitored and frequently audited areas in 2026. CMS and Medicare Administrative Contractors (MACs) are tightening oversight due to rising concerns around maintenance care billing, repetitive treatment patterns, and weak clinical documentation.
Medicare only reimburses chiropractic services when spinal manipulation is performed to correct a documented spinal subluxation. Coverage remains limited and heavily dependent on strong medical necessity support.
Medicare generally does not cover:
- Maintenance or long-term wellness care
- Routine adjustments without clinical improvement
- Massage therapy services
- X-rays for billing purposes only
- Acupuncture without proper credentialing
Because of these restrictions, providers must clearly prove that care is active, corrective treatment, not ongoing maintenance.
To support reimbursement, documentation must clearly include:
- Medical necessity justification
- Functional improvement goals
- Objective clinical findings
- Active treatment plans
- Ongoing reassessment
- Measurable patient progress
Without strong documentation, claims may be denied even if CPT coding is correct.
Chiropractic CPT Codes in 2026
The following chiropractic CPT codes remain among the most commonly billed procedures under Medicare and commercial insurance plans:
| CPT Code | Description |
| 98940 | Chiropractic manipulative treatment involving 1–2 spinal regions |
| 98941 | Chiropractic manipulative treatment involving 3–4 spinal regions |
| 98942 | Chiropractic manipulative treatment involving 5 spinal regions |
Although these codes remain stable, payer scrutiny surrounding treatment frequency, documentation quality, and spinal region justification continues increasing.
Insurance carriers now compare diagnosis coding, treatment patterns, and progress documentation across multiple visits to identify repetitive or unsupported care plans.
Understanding the AT Modifier in Chiropractic Billing
The AT modifier remains one of the most important requirements in Medicare chiropractic billing.
This modifier confirms that treatment represents active or corrective care instead of maintenance therapy. Claims submitted without the AT modifier are often automatically denied because Medicare assumes the service is maintenance-based.
However, simply adding the modifier is not enough. Documentation must clearly support medical necessity throughout the patient’s treatment plan.
Providers should document:
- Subluxation findings
- Functional impairments
- Pain severity
- Objective examination findings
- Treatment goals
- Patient progress
- Reassessment results
Medicare auditors increasingly review whether documentation demonstrates measurable improvement over time. Repetitive treatment notes or vague progress descriptions can increase audit risk significantly.
Increased Chiropractic Audit Activity
CMS continues increasing chiropractic audit activity across the United States, especially in states with historically high chiropractic utilization rates such as Florida, Texas, California, Michigan, and Illinois.
Many providers are now facing:
- Targeted Probe and Educate (TPE) reviews
- Recovery Audit Contractor (RAC) audits
- Documentation requests
- Post-payment reviews
- Utilization investigations
AI-assisted Medicare review systems are becoming increasingly advanced and can now identify repetitive treatment patterns, unsupported diagnosis combinations, excessive visit frequency, and modifier inconsistencies much faster than traditional manual reviews.
Physical Therapy Billing Challenges in 2026
Physical therapy billing continues becoming more complicated due to timed coding rules, authorization requirements, therapy threshold monitoring, and payer-specific documentation standards.
Physical therapy practices must carefully manage:
- Timed CPT coding compliance
- Plan of care documentation
- Authorization renewals
- Progress note requirements
- Functional outcome reporting
- Medical necessity validation
- Modifier compliance
Even experienced providers struggle because reimbursement requirements vary significantly between Medicare, Medicaid, workers’ compensation carriers, and commercial insurance plans.
As payer review systems become increasingly automated, documentation accuracy is more important than ever.
Common Physical Therapy CPT Codes in 2026
The following CPT codes are among the most frequently billed physical therapy procedures:
| CPT Code | Description |
| 97110 | Therapeutic exercises |
| 97112 | Neuromuscular reeducation |
| 97116 | Gait training therapy |
| 97140 | Manual therapy |
| 97530 | Therapeutic activities |
| 97535 | Self-care and home management training |
Many of these procedures involve timed billing requirements, creating additional compliance challenges for rehabilitation providers.
Insurance carriers increasingly compare billed units against documented treatment minutes using AI-assisted review systems.
Medicare 8-Minute Rule (PT Billing)
| Time | Units |
| 8–22 min | 1 unit |
| 23–37 min | 2 units |
| 38–52 min | 3 units |
Incorrect time documentation is now one of the most common automated denial triggers in PT billing systems.
Medicare Therapy Threshold & KX Modifier Updates
Physical therapy billing compliance extends beyond CPT coding accuracy. Medicare continues closely monitoring outpatient therapy utilization, especially when treatment exceeds annual therapy thresholds.
Once therapy services exceed Medicare’s designated threshold amount, providers must append the KX modifier to confirm that continued treatment remains medically necessary.
Documentation should include:
- Functional outcome measurements
- Updated treatment goals
- Objective reassessment findings
- Skilled intervention justification
- Progress toward recovery
CMS continues increasing review activity for high-utilization rehabilitation claims, making accurate documentation essential for reimbursement protection.
ICD-10 Coding Requirements for Chiropractic & PT Billing
ICD-10 specificity plays a major role in reimbursement approval because payers evaluate whether diagnosis codes properly support medical necessity for billed procedures.
Generalized pain diagnoses often trigger additional review or reimbursement reductions.
Common chiropractic ICD-10 diagnosis codes include:
| ICD-10 Code | Description |
| M99.01 | Segmental dysfunction of cervical region |
| M99.03 | Segmental dysfunction of lumbar region |
| M54.2 | Cervicalgia |
| M54.5 | Low back pain |
Common physical therapy ICD-10 diagnosis codes include:
| ICD-10 Code | Description |
| M25.561 | Pain in right knee |
| M62.81 | Muscle weakness |
| R26.2 | Difficulty walking |
| S83.511A | Sprain of right ACL |
Accurate diagnosis coding helps support medical necessity while reducing denials and audit exposure.
Important Modifier Usage Beyond AT
Modifier compliance remains one of the largest challenges in chiropractic and physical therapy billing.
Several modifiers play critical roles in reimbursement approval:
| Modifier | Purpose |
| AT | Active treatment |
| GP | Services delivered under PT plan of care |
| KX | Medical necessity threshold exceeded |
| 59 | Distinct procedural service |
| CQ | PTA services |
| CO | OTA services |
Incorrect modifier usage frequently results in automated denials, payment delays, or audit reviews.
Because payer rules vary significantly, practices must carefully monitor modifier requirements across all insurance plans.
Prior Authorization Challenges in Physical Therapy Billing
Prior authorization remains one of the largest administrative burdens for physical therapy providers in 2026.
Commercial insurance carriers increasingly require authorization approvals before therapy services begin, particularly for long-term rehabilitation programs and post-surgical treatment plans.
Many practices struggle with:
- Delayed authorization approvals
- Visit limitation tracking
- Authorization expirations
- Retroactive authorization denials
- Payer-specific authorization rules
States such as California, Texas, Florida, and New York continue experiencing particularly strict authorization oversight from commercial payers.
As payer requirements become more complex, many rehabilitation providers are adopting AI-assisted authorization tracking systems to monitor visit counts and payer rules more efficiently.
Essential Documentation Requirements
Strong documentation remains the foundation of successful chiropractic and physical therapy reimbursement in 2026.
Insurance carriers and Medicare reviewers increasingly analyze treatment records to determine whether services are medically necessary and properly supported by objective findings.
Essential documentation elements include:
- Initial evaluations
- Functional limitation assessments
- Daily treatment notes
- Objective progress measurements
- Reassessment documentation
- Updated treatment goals
- Discharge summaries
For chiropractic providers, documentation should clearly support spinal subluxation findings, functional impairment, and active corrective treatment goals.
For physical therapy providers, treatment records should demonstrate measurable patient improvement and skilled therapeutic intervention.
Generic or repetitive treatment templates may increase audit risk because AI-assisted payer systems can now identify cloned documentation patterns more efficiently.
Telehealth & Remote Therapeutic Monitoring Trends
Telehealth and Remote Therapeutic Monitoring (RTM) continue expanding across rehabilitation specialties in 2026.
Many providers now use digital monitoring tools to track home exercise adherence, mobility progression, pain levels, and recovery outcomes outside traditional clinic visits.
RTM services are becoming increasingly common for:
- Orthopedic rehabilitation
- Post-surgical recovery
- Chronic pain management
- Neurological rehabilitation
- Sports injury recovery
However, billing compliance remains challenging because Medicare and commercial payer policies continue evolving.
Providers must carefully document patient consent, device usage data, monitoring activities, and communication time to support reimbursement.
Medicare vs Commercial Payer Billing Differences
One of the biggest challenges for chiropractic and physical therapy providers is managing different payer requirements simultaneously.
| Billing Area | Medicare | Commercial Insurance |
| AT Modifier | Required for active chiropractic treatment | Varies by payer |
| Authorization Requirements | Limited in many cases | Frequently required |
| Visit Limits | Threshold-based monitoring | Plan-specific limitations |
| Documentation Standards | CMS guidelines | Payer-specific rules |
Because payer expectations vary significantly, rehabilitation providers must maintain highly organized billing workflows to avoid denials and compliance risks.
The Financial Impact of Claim Denials
Claim denials continue creating major financial pressure for rehabilitation providers nationwide.
Industry estimates suggest that healthcare denial rates average between 5% and 10%, while nearly 60% of denied claims are never successfully reworked. For chiropractic and physical therapy practices, even small billing inefficiencies can create significant long-term revenue leakage.
Authorization failures, modifier errors, documentation gaps, and coding inconsistencies remain among the leading causes of reimbursement loss.
Denied claims also increase administrative workload because staff must spend additional time on:
- Claim corrections
- Appeals
- Payer follow-up calls
- Medical record requests
- Claim resubmissions
As reimbursement pressure increases, proactive denial prevention is becoming far more cost-effective than reactive denial management.
Proactive Denial Prevention Workflow for 2026
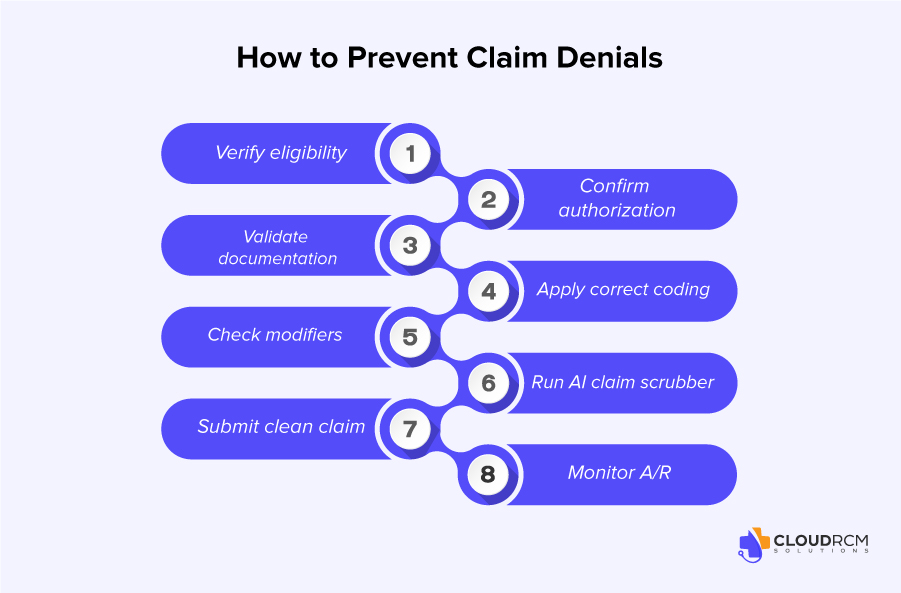
Successful rehabilitation organizations are increasingly adopting proactive denial prevention strategies instead of reacting after claims are denied.
A modern denial prevention workflow typically includes:
- Insurance eligibility verification
- Prior authorization validation
- Documentation quality review
- CPT and ICD-10 coding validation
- Modifier compliance checks
- AI-assisted claim scrubbing
- Real-time denial trend monitoring
- Accounts receivable follow-up analytics
This proactive approach helps providers reduce claim rework, improve clean claim rates, accelerate reimbursements, and strengthen compliance performance.
How AI Is Transforming Chiropractic & PT Billing
Artificial intelligence is rapidly reshaping revenue cycle management for rehabilitation providers in 2026.
Modern AI-assisted billing systems can:
- Detect coding inconsistencies before claim submission
- Identify denial trends in real time
- Monitor modifier compliance
- Predict reimbursement risks
- Track authorization deadlines
- Improve clean claim rates
- Reduce manual billing errors
AI-driven systems also help practices identify operational weaknesses before major revenue loss occurs.
However, technology alone cannot eliminate denials completely. Successful organizations combine AI automation with experienced medical billing professionals who understand specialty-specific payer regulations and compliance requirements.
How Cloud RCM Solutions Supports Chiropractic & PT Practices
Cloud RCM Solutions provides specialized revenue cycle management services for chiropractic clinics, physical therapy providers, orthopedic rehabilitation groups, sports medicine practices, pain management organizations, and outpatient therapy centers.
Using AI-assisted billing technology and specialty-focused RCM expertise, Cloud RCM Solutions helps providers:
- Reduce chiropractic and PT claim denials
- Improve clean claim submission rates
- Strengthen Medicare compliance workflows
- Optimize authorization management
- Improve reimbursement accuracy
- Accelerate accounts receivable recovery
- Monitor payer trends and audit risks
- Enhance long-term cash flow stability
Rather than offering generic billing support, Cloud RCM Solutions develops customized revenue cycle strategies based on each practice’s specialty, payer mix, and financial goals.
Final Thoughts
Chiropractic and physical therapy billing in 2026 is more complex due to evolving CPT rules, stricter ICD-10 requirements, Medicare regulations, modifier compliance, AI-based claim reviews, and rising audit activity. Even minor billing errors can significantly impact reimbursements.
For chiropractic clinics, physical therapy providers, orthopedic rehab groups, and sports medicine practices, financial stability now depends on accurate documentation, strong compliance, and proactive denial management.
Cloud RCM Solutions supports rehabilitation providers with AI-driven billing, Medicare compliance expertise, denial prevention, and specialty-focused revenue cycle management to improve reimbursements in 2026.
FAQs
What is the AT modifier in chiropractic billing?
The AT modifier indicates that chiropractic treatment represents active corrective care rather than maintenance therapy.
Does Medicare cover chiropractic adjustments in 2026?
Yes, Medicare covers medically necessary spinal manipulation services used to correct documented subluxation conditions.
What is the KX modifier used for in physical therapy billing?
The KX modifier confirms that therapy services exceeding Medicare thresholds remain medically necessary and properly documented.
Why are PT claims denied in 2026?
Physical therapy claims are commonly denied because of authorization failures, modifier errors, insufficient documentation, and coding inaccuracies.therapy claims are commonly denied because of authorization failures, modifier errors, insufficient documentation, and coding inaccuracies.

 Medical Billing
Medical Billing Medical Coding
Medical Coding Medical Audit
Medical Audit Provider Credentialing
Provider Credentialing Denial Management
Denial Management A/R Follow-up
A/R Follow-up Private Practice
Private Practice Patient Help Desk
Patient Help Desk Customized Reporting
Customized Reporting Out-of-Network Billing
Out-of-Network Billing Internal Medicine
Internal Medicine Pediatrics
Pediatrics Radiology
Radiology Surgery
Surgery Emergency Medicine
Emergency Medicine Anesthesiology
Anesthesiology Cardiology
Cardiology Orthopedic
Orthopedic Psychiatry
Psychiatry Dentistry
Dentistry OB-GYN
OB-GYN Family Medicine
Family Medicine


