The 2026 Medicare Physician Fee Schedule (PFS) is reshaping how Internal Medicine practices manage billing and reimbursement. While federal rules provide a baseline, state-specific Medicare policies, including Local Coverage Determinations (LCDs) and regional documentation requirements, can significantly affect revenue and operational workflows.
For Internal Medicine providers managing chronic conditions, preventive care, and telehealth services, understanding these state-level variations is essential to maximize reimbursement, reduce denials, and maintain compliance.
Why State-Specific Medicare Rules Matter for Internal Medicine
Internal Medicine practices are heavily reliant on Medicare revenue, particularly for chronic care management (CCM), evaluation and management (E/M) services, and preventive care. State-specific rules influence how services are billed and reimbursed:
- Reimbursement Differences: States may adjust payment rates for CCM, telehealth, and preventive services differently, creating revenue variation even under the same federal PFS.
- Documentation Requirements: Some states require stricter clinical notes, time tracking, and patient engagement documentation, particularly for chronic care and telehealth.
- Prior Authorization Rules: Certain procedures, labs, or imaging may require state-specific pre-approvals or modifiers to qualify for reimbursement.
- Audit Patterns: Regional Medicare contractors may prioritize audits on services or specialties based on local patterns and spending trends.
Even minor differences between states can lead to underpayments, delayed revenue, and compliance risk for practices serving multi-state patient populations.
Key Challenges for Internal Medicine Practices Under the 2026 PFS
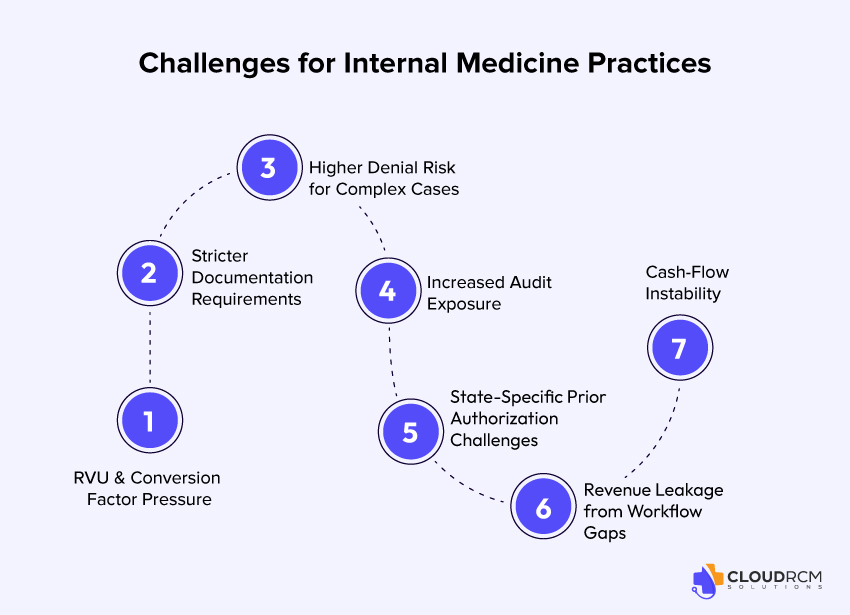
Internal Medicine practices face several challenges under the 2026 PFS, compounded by state-level variations:
- RVU & Conversion Factor Pressure
Payments for E/M and chronic care services are calculated using Relative Value Units (RVUs). With 2026 adjustments, even small reductions per service can accumulate over high patient volumes, impacting total revenue.
- Stricter Documentation Requirements
States may require additional documentation for CCM, preventive visits, and telehealth. Missing time-tracking, clinical notes, or engagement details can trigger denials or underpayments.
- Higher Denial Risk for Complex Cases
Internal Medicine providers managing patients with multiple chronic conditions face increased scrutiny. Improperly coded visits, missing modifiers, or incomplete documentation frequently lead to claim denials.
- Increased Audit Exposure
Regional Medicare contractors target high-volume or high-reimbursement services for audits. Practices without precise, state-compliant documentation may face recoupments and penalties.
- State-Specific Prior Authorization Challenges
Labs, imaging, and telehealth services may require state-specific pre-approvals. Missing these approvals can result in delayed payment or claim rejection.
- Revenue Leakage from Workflow Gaps
Fragmented coordination between clinical and billing teams often leads to missed charges, underbilled preventive services, or unrecorded chronic care visits, accumulating as invisible revenue losses.
- Cash-Flow Instability
Denials, delayed payments, and underpayments create unpredictable monthly revenue, affecting payroll, vendor payments, and operational planning.
State-Specific Impacts on Internal Medicine Practices
Chronic Care Management (CCM) & E/M Services
- High Medicare Reliance: CCM and E/M visits are central to Internal Medicine revenue streams.
- State Variations: Some states enforce stricter documentation or reporting for CCM and transitional care management (TCM).
- Impact: Missing state-specific documentation or failing to report proper time can lead to denials or reduced reimbursement.
Preventive Care & Screening
- Screening Requirements: Annual wellness visits, labs, and preventive services may vary in coverage by state.
- Impact: Failure to comply with state-specific documentation or modifier requirements can lead to delayed or denied claims.
Telehealth & Virtual Care
- Post-Pandemic Policies: Telehealth coverage rules differ by state, with some limiting eligible services or requiring additional documentation, prior authorization, or specific coding for payment.
- Impact: Practices unaware of local telehealth policies risk losing revenue on virtual visits and potential claim rejections.
State-Specific Medicare Variations Table
| State | Chronic Care Management (CCM) | Preventive Care / Wellness Visits | Telehealth / Virtual Care | Key Notes |
| California | Requires detailed time logs for CCM; separate billing for multiple chronic conditions | Modifier usage required for annual wellness visits | Expanded telehealth coverage through 2026 | High documentation scrutiny; proactive audits common |
| Texas | CCM billing allowed only if minimum 20 min/month documented | Preventive visits reimbursed at standard federal rates | Telehealth limited to select services | Prior authorization required for some labs/imaging |
| Florida | CCM reimbursement allowed for up to 2 chronic conditions per patient | Preventive screenings may require state-specific codes | Telehealth covered broadly for primary care | Focus on chronic condition justification |
| New York | CCM documentation must include care plan and patient engagement notes | Annual wellness visits require E/M code alignment | Telehealth reimbursement follows federal guidelines | Higher denial risk without proper documentation |
| Illinois | CCM claims require confirmation of patient consent | Preventive visits follow federal PFS but require state modifier for telehealth | Some post-pandemic telehealth flexibilities rolled back | Multi-state practices must track LCD differences |
| Georgia | Limited CCM reimbursements for multiple providers | Preventive care follows federal PFS | Telehealth limited to evaluation and management visits | Audit exposure increases if documentation incomplete |
Multi-state Internal Medicine practices must maintain compliance in each jurisdiction to avoid revenue loss.
Actionable RCM Strategies for Internal Medicine Practices
To navigate state-specific Medicare rules and safeguard revenue, Internal Medicine practices should adopt a proactive, data-driven revenue cycle management approach:
- Comprehensive Charge Capture Audits: Review E/M, CCM, and preventive service codes to ensure all billable services are captured.
- Integrated Documentation Workflows: Align clinical notes with state-specific billing rules to reduce denials and audit exposure.
- Proactive Denial Management: Implement real-time denial tracking, root-cause analysis, and appeal processes for high-risk claims.
- Prior Authorization & Eligibility Checks: Verify approvals for labs, imaging, and telehealth services per state requirements.
- Staff Training on State-Specific Rules: Educate clinical and billing staff on local Medicare policies and documentation standards.
- Financial Forecasting & Cash-Flow Monitoring: Model revenue based on state-specific PFS adjustments to anticipate potential shortfalls.
- Multi-State Oversight: Monitor LCDs and state-specific coverage variations for multi-location practices to maintain compliance and reimbursement consistency.
Implementing these strategies allows Internal Medicine practices to reduce denials, recover lost revenue, and maintain operational stability under 2026 Medicare rules.
Why Medicare-Focused RCM Is Essential for Internal Medicine Practices in 2026
The 2026 Medicare Physician Fee Schedule, combined with state-specific variations, has changed the way Internal Medicine practices must manage billing and revenue. Medicare-focused revenue cycle management is no longer optional; it is a strategic necessity to protect reimbursement, reduce denials, and maintain financial stability across multi-state operations.
Cloud RCM Solutions helps Internal Medicine practices navigate these challenges by providing targeted, specialty-focused RCM strategies that align with federal and local Medicare rules.
How Cloud RCM Solutions Helps Practices Navigate 2026 Medicare Challenges
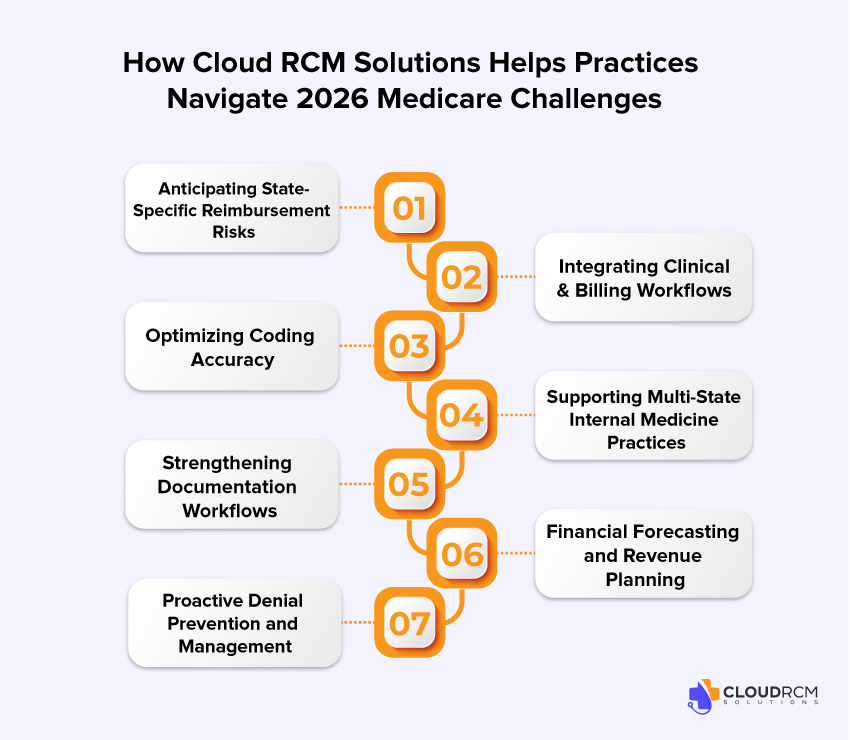
Cloud RCM Solutions helps your practice stay ahead by forecasting revenue risks, optimizing coding accuracy, strengthening documentation, and preventing denials before they impact cash flow. We seamlessly connect clinical and billing workflows, support multi-state compliance, and deliver smart financial insights so you can maximize reimbursements, reduce revenue leakage, and keep your practice financially strong in an ever-changing healthcare landscape.
Conclusion
The 2026 Medicare Physician Fee Schedule, combined with state-specific rules, presents new challenges and risks for Internal Medicine practices. From chronic care management to preventive services and telehealth, revenue loss, denials, and compliance issues are real threats without a proactive RCM strategy.
Schedule a consultation today to review your Internal Medicine billing workflows, implement state-compliant strategies, and protect your practice’s financial health in 2026 and beyond.
FAQ’s
How do state-specific rules affect Medicare billing for Internal Medicine?
State-specific Local Coverage Determinations (LCDs) and documentation requirements can impact reimbursement, prior authorization, and audit risk for CCM, preventive visits, and telehealth services.
What are the biggest challenges Internal Medicine practices face under the 2026 Medicare PFS?
Challenges include RVU compression, stricter documentation, higher denial risk, audit exposure, prior authorization requirements, and revenue leakage from workflow gaps.
How can Internal Medicine practices optimize CCM billing under state-specific rules?
By documenting care plans, tracking patient engagement time, verifying prior authorizations, and aligning with state LCDs, practices can reduce denials and maximize CCM reimbursement.
Do preventive care visits vary by state for Medicare billing?
Yes. States may require different modifiers, documentation, or billing codes for annual wellness visits and preventive screenings, affecting reimbursement and compliance.
How is telehealth billing affected by state rules in 2026?
Telehealth coverage varies by state, with some limiting eligible services or requiring additional documentation, prior authorization, or specific coding for payment.
What is the impact of denied CCM or preventive claims on Internal Medicine practices?
Denials create delayed revenue, disrupt cash flow, and increase administrative burden, particularly for high-volume chronic care and preventive service providers.
Why is multi-state oversight important for Internal Medicine practices?
Practices operating in multiple states must track state-specific Medicare rules, LCDs, and prior authorization requirements to maintain consistent compliance and revenue.
How can proactive denial management help Internal Medicine practices?
By analyzing root causes, tracking claims in real time, and appealing high-risk denials, practices can recover revenue and reduce delays in cash flow.
What role does documentation play in reducing audit exposure for Internal Medicine practices?
Proper, state-compliant documentation ensures CCM, E/M, and preventive visits are audit-ready, reducing the risk of recoupment or penalties.
How can Internal Medicine practices stay financially stable under 2026 Medicare rules?
Adopting a data-driven RCM approach, conducting charge audits, monitoring multi-state regulations, and aligning clinical and billing workflows help practices maintain revenue and operational stability.

 Medical Billing
Medical Billing Medical Coding
Medical Coding Medical Audit
Medical Audit Provider Credentialing
Provider Credentialing Denial Management
Denial Management A/R Follow-up
A/R Follow-up Private Practice
Private Practice Patient Help Desk
Patient Help Desk Customized Reporting
Customized Reporting Out-of-Network Billing
Out-of-Network Billing Internal Medicine
Internal Medicine Pediatrics
Pediatrics Radiology
Radiology Surgery
Surgery Emergency Medicine
Emergency Medicine Anesthesiology
Anesthesiology Cardiology
Cardiology Orthopedic
Orthopedic Psychiatry
Psychiatry Dentistry
Dentistry OB-GYN
OB-GYN Family Medicine
Family Medicine


