Medical billing and coding services are vital elements of the healthcare industry, functioning as the essential link between you as a healthcare provider, your patients, and insurance companies.
Medical billing and coding services are vital elements of the healthcare industry, functioning as the essential link between you as a healthcare provider, your patients, and insurance companies. These services are critical in ensuring accurate healthcare coding and the subsequent compensation for the services you provide.

Medical billing is the process by which your services are submitted and followed up on with health insurance companies, leading to the receipt of payment for your services. Essentially, it involves translating the healthcare services you’ve rendered into billable claims, which are then forwarded to insurance companies for payment.
Conversely, coding is the process of applying standardized codes to the medical diagnoses, procedures, and treatments that you perform. This critical step translates the narrative of a patient’s condition and the healthcare services provided into a universal language that is understood and processed by both the healthcare system and insurance companies.
Understanding medical billing and coding services is crucial not just for smooth administrative functioning, but also for ensuring compliance with legal and regulatory requirements. Accurate billing and coding practices can safeguard your practice against audits, prevent errors leading to claim denials, and contribute to the overall financial health of your practice.
Are you ready to delve deeper into the world of medical billing and coding? Understanding the fundamental steps involved in these processes can streamline your healthcare practice, making it more efficient and effective.
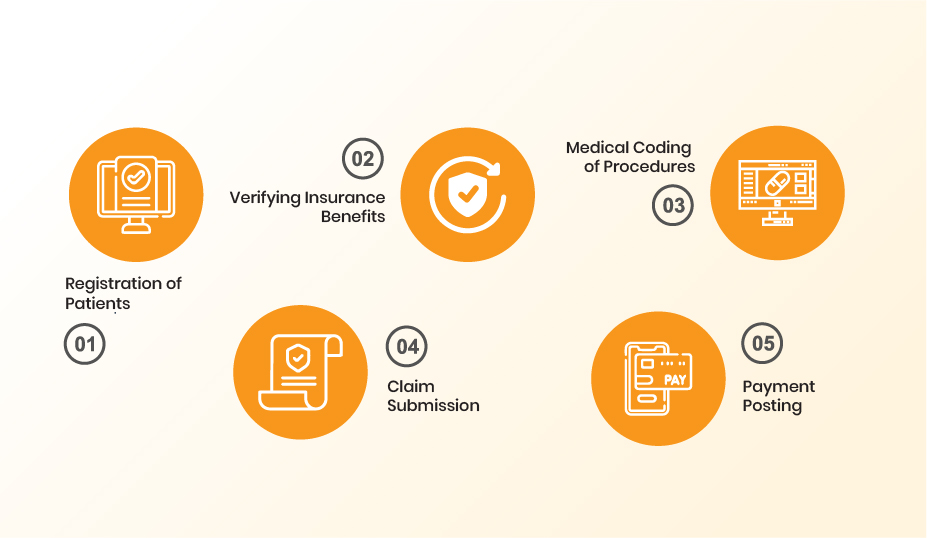
The first crucial step involves registering new patients when they visit your healthcare practice for the first time. During this step, you’ll collect necessary information like the patient’s full name, date of birth, contact details, and insurance information.
Before providing medical services, it’s essential that you verify the patient’s insurance eligibility and benefits. This step involves confirming the insurance details provided, checking the coverage benefits, deductibles, co-payment, and confirming whether the planned services are covered under the patient’s policy.
After the patient’s visit, you’ll translate the services provided, diagnoses made, and any procedures performed into standardized medical codes. This coding process, using systems like ICD (International Classification of Diseases) and CPT (Current Procedural Terminology), allows for universal understanding and processing of healthcare services.
Once the services have been accurately coded, you’ll prepare and submit the claim to the patient’s insurance company. This claim includes the patient’s personal and insurance information, along with the details of the services provided, all encoded in the universally accepted medical coding language.
The final step in the process involves posting the payments received from the insurance company and the patient. If there are delays or issues with the payment, your role includes following up with the insurance company, and if necessary, submitting an appeal for denied or underpaid claims.
Are you curious about the training necessary to successfully pursue medical billing and coding? It’s crucial to have a solid educational foundation and hands-on training to competently perform these services.
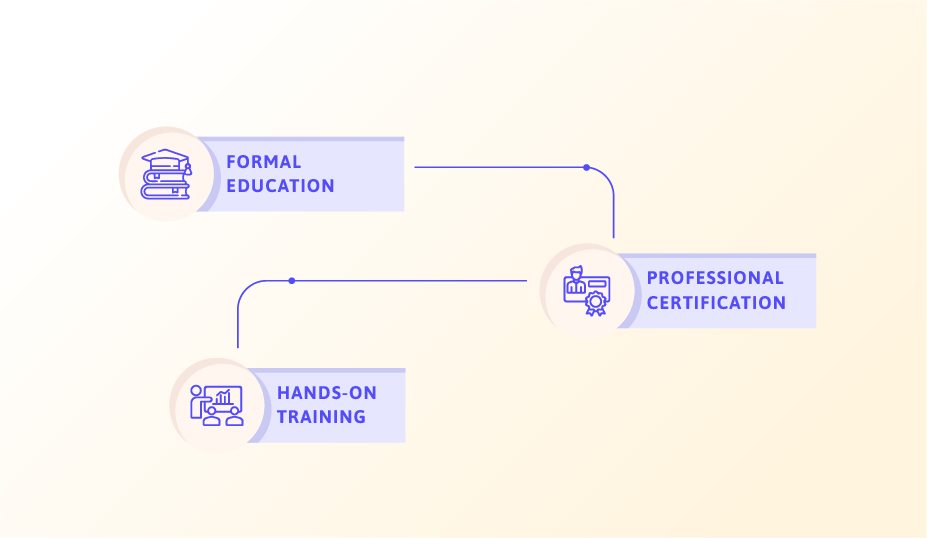
The journey towards becoming a proficient medical billing and coding specialist begins with acquiring a high school diploma or its equivalent. However, to increase your employability, you should consider further education such as diploma programs, associate’s degrees, or certificate programs in medical billing and coding.
Upon completing your education, it’s highly beneficial to earn professional certifications, like the Certified Professional Coder (CPC) or Certified Coding Specialist (CCS). These certifications demonstrate your competency and commitment to maintaining a high standard of proficiency in the field.
Practical experience is invaluable in this field. You may get this through internships, on-the-job training, or experiential learning components of a formal education program, all of which help you understand the real-world application of medical billing and coding.
When you implement medical billing and coding services, it is no surprise that you may encounter many unprecedented challenges. These challenges, while potentially daunting, can serve as learning opportunities to improve your proficiency and skill set.
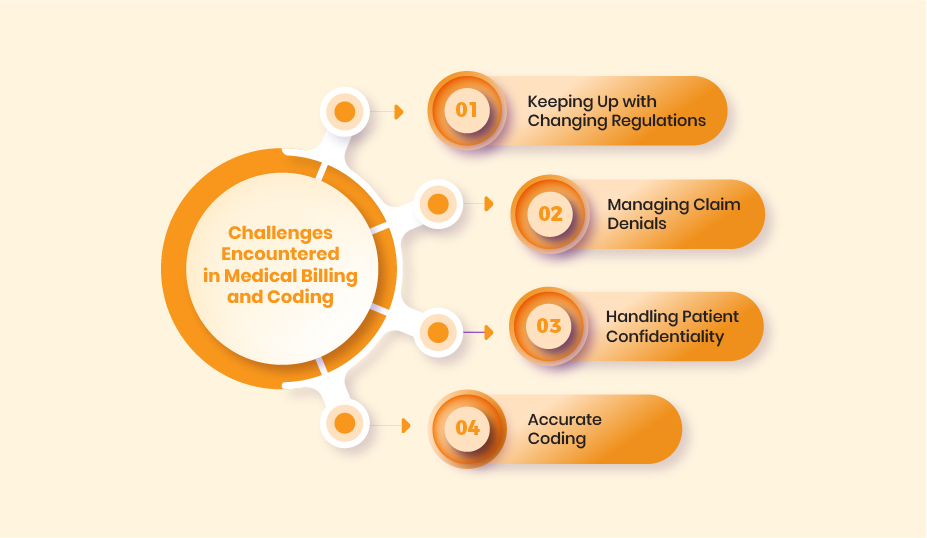
The medical billing and coding industry is governed by numerous regulations that are subject to frequent changes. Keeping abreast with these updates can be quite a challenge. Failure to stay updated can lead to errors in coding, claim denials, or potential legal issues. Therefore, continuous learning and adaptation are paramount in this field.
Despite best efforts, claim denials from insurance companies are a common issue in medical billing. This can be due to a multitude of reasons, including coding errors, missing information, or issues with the insurance policy. Successfully managing and reducing these denials requires careful attention to detail, a thorough understanding of insurance guidelines, and persistent follow-up.
Handling sensitive patient information is a core aspect of medical billing and coding. Ensuring that this data remains confidential can be challenging, particularly in our digital age. You must adhere to strict guidelines and regulations, such as the Health Insurance Portability and Accountability Act (HIPAA), to safeguard patient information and prevent any breaches of confidentiality.
Accurate coding is crucial to ensure appropriate billing and reimbursement. However, with thousands of codes and regular updates to coding systems like ICD and CPT, maintaining accuracy can be a challenging task. Ongoing training and meticulous attention to detail are essential to master this aspect of the job.
Considering the challenges associated with medical billing and coding, outsourcing these services is an option that can yield considerable benefits. It can offer solutions to many of the challenges and problems that you might not be able to resolve fully.
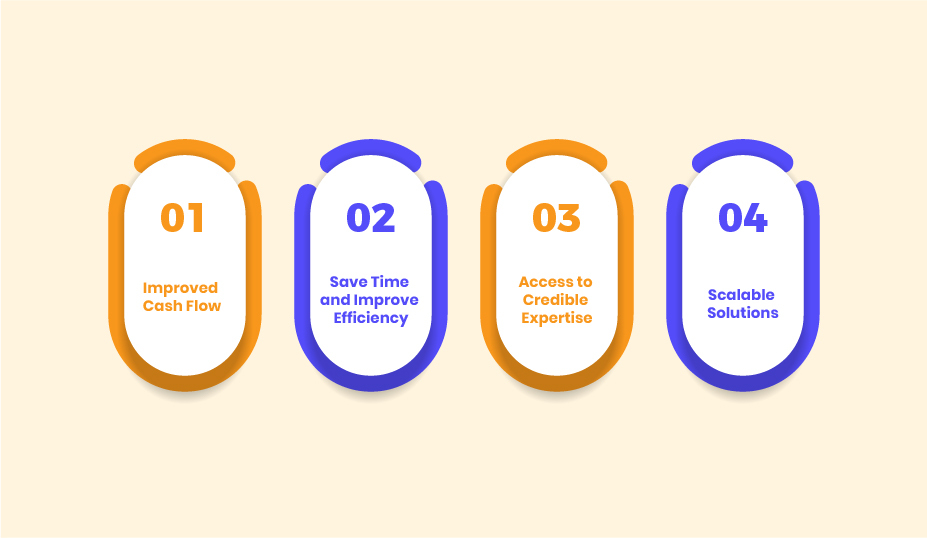
With a dedicated team handling your billing and coding, claims are processed more quickly and accurately. This can lead to faster reimbursement from insurance companies, thereby improving your cash flow. In addition, they can handle patient billing inquiries, freeing your staff from these time-consuming tasks.
Outsourcing these services can free up substantial amounts of time for your practice. Instead of spending time on administrative tasks like billing and coding, you and your staff can focus more on patient care. This allows you to better utilize your expertise and improves overall efficiency.
Outsourcing companies specialize in medical billing and coding, meaning they have extensive knowledge and stay up-to-date with changes in regulations and codes. This expertise leads to fewer coding errors and claim denials, ensuring you receive accurate reimbursement. Furthermore, these companies use the latest technology and follow best industry practices, adding another layer of reliability.
As your practice grows, so do your billing and coding needs. Outsourcing these services offers scalability without the need to hire more staff or expand your office space. This means you can effortlessly handle an increase in patients or services, making it easier to grow your practice.
Medical billing and coding services must adhere to numerous regulations, including the Health Insurance Portability and Accountability Act (HIPAA) and the False Claims Act. Failing to comply can result in significant legal consequences, such as fines and potential lawsuits. Therefore, it’s crucial that you stay current with these laws and ensure that your practice is fully compliant.
Given the complexity and the constant updates to the coding systems, the potential for coding errors is quite high. Such mistakes can lead to incorrect billing, claim denials, and potential legal issues. Attention to detail, ongoing training, and double-checking your work are essential to minimizing these errors.
Handling sensitive patient data comes with the responsibility of maintaining data security. A breach in data security could compromise patient confidentiality, leading to legal issues and loss of trust from patients. Therefore, it’s essential that you have robust data security measures in place and remain vigilant about potential threats.
Errors in billing and coding can lead to underpayment or non-payment of claims from insurance companies. This could have a significant impact on your practice’s revenue and cash flow. Regular audits and quality checks can help ensure accuracy in billing and coding, thereby reducing these issues.
As you look towards the future, the medical billing and coding field is poised for some significant developments. Technological advancements and healthcare reform will continue to shape this industry, presenting both opportunities and challenges. Here’s what you can expect.
The rise of Artificial Intelligence (AI) and machine learning will likely streamline the billing and coding processes, reducing the likelihood of errors and increasing efficiency. These technologies can automate many routine tasks, freeing up your time to focus more on patient care. However, this automation could also necessitate the need for advanced technical skills to manage these systems.
Regulatory changes will continue to be a key aspect of the future of medical billing and coding. As healthcare policies evolve, you’ll need to stay updated to ensure compliance and accurate reimbursement. Continued education and adaptability will remain crucial to navigate these changes and continue providing high-quality care to your patients.
To sum it up, the field of medical billing and coding is a fundamental pillar of the healthcare industry. Whether it is the steps involved, risks, challenges or other aspects, comprehending the insights of medical billing and coding is of undeniable importance for a successful healthcare business.
At CloudRCM Solutions, we excel in providing superior medical billing and coding services. With our expert team staying ahead with the changing regulations and leveraging the latest technology, we ensure that your healthcare business runs smoothly, stays compliant, and maximizes its financial health. Contact us today and integrate the best medical billing and coding services for your business.

Revenue Cycle Management (RCM), the method for handling healthcare claims adjudication, is the revenue generator for